Emergency Room and Urgent Care Providers
How to deal with the patient who presents with a pilonidal abscess?
Frequently a pilonidal patient’s first contact with the healthcare system is in an emergency room or urgent care clinic. Often, this experience is sub-optimal. Social media is rife with patient complaints about how they were treated (or not treated) in the emergency setting. This web page discusses successful strategies for clinicians dealing with this, and in particular dealing with the patient who presents with an acute pilonidal abscess.
Patients do not present to an ER with pain in the gluteal crease unless it is pretty severe. Although physical findings may be minimal, this should be taken seriously, with the understanding that it is your job to help the patient solve this problem quickly and successfully.
First, it is important to make a diagnosis. Acute pain in the gluteal crease is usually a pilonidal abscess until proven otherwise. Other less common possibilities are hidradenitis suppurativa (HS) or an infected sebaceous cyst, the former can usually be determined by history, and the latter being very unlikely in that particular location. In the perianal region the diagnosis can be confused with a perirectal abscess, but the location will usually exclude one or the other to an experienced clinician.
The treatment of a pilonidal abscess is surgical drainage!
If you suspect that a patient has a pilonidal abscess, surgical drainage should be at the forefront of your treatment algorithm. Sending the patient home with antibiotics may seem like a good strategy because it is simple, non-traumatic, inexpensive, and gets the patient out of the ER and on their way quickly. But, it is usually not the solution to their problem.
I will discuss various scenarios below:
What if the abscess has already started to drain?
If the abscess is already self-draining, and the drainage seems adequate – local wound care, antibiotics, and referral to a surgeon in a couple of weeks is quite reasonable. The purpose of the surgeon referral would be to discuss more permanent ways to treat pilonidal disease. It will help the patient for you to provide them with a diagnosis, so they understand what is happening. If the drainage is just coming through a tiny opening, enlarging that opening is a good idea, otherwise the patient may be back in the ER in a day or two complaining of the same problem.
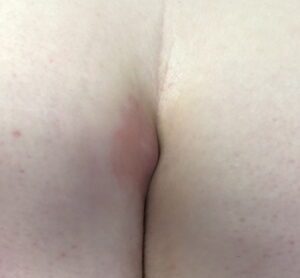
What if it is obvious where to drain the abscess?
If it is fluctuant and close to the surface, drainage under local anesthesia in the ER is reasonable. However, the patient’s personality, pain threshold, and personal preferences should be taken into account. If it doesn’t seem that drainage under local anesthesia is going to go well, the next option is to provide a solution that will make the patient comfortable during the drainage procedure. This usually means contacting a surgeon to take the patient to an operating or procedure room that is staffed with anesthesia for surgical drainage.
This may seem like a lot of rigamarole to go through for a very simple drainage procedure – but I believe that our goal is to solve this problem in the least traumatic way possible. Although this may be a significantly more expensive option, patients are very grateful, and I have yet to have one complain about the cost.
How to drain a pilonidal abscess
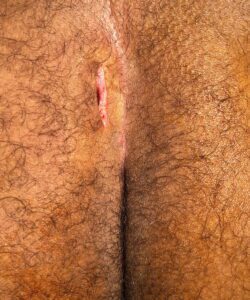
When draining a pilonidal abscess in the ER or the OR it is very important that the site of drainage be off the midline and out of the gluteal fold. Local anesthetic with epinephrine should be used to minimize bleeding.
It is also important that the incision be long enough to accomplish adequate drainage: 1-2 centimeters is the minimal adequate length. A small 5mm slit will frequently close up and the abscess may recur.
It is NOT necessary to place any kind of packing into the abscess cavity. These abscesses should be drained, and covered with a dry dressing. (The only time I would pack a pilonidal abscess would be if the interior cavity walls were bleeding so much that internal pressure from the gauze was needed to stop the bleeding.)
What if you suspect an abscess, but there are minimal external signs?
This is a very common scenario, and often these patients are sent home on antibiotics with hopes that the abscess will resolve or will self drain. This is often an inadequate approach. These patients need surgical drainage with general anesthesia or sedation, and it is your job to arrange this in a timely fashion. This is one of the most common complaints seen on social media as patients discuss their ER care.
The optimal situation is that you see the patient, determine that drainage is needed, call up your local surgeon, he sees the patient today, and arranges a drainage procedure for today or tomorrow (depending on the schedule and when the patient has last eaten). Unfortunately, this scenario is rarely the case. But nonetheless, some attempt should be made to have the patient seen in a timely manner for drainage. It is reasonable to start antibiotics right away. Studies show that most of these abscesses contain anaerobes along with some gram (-) rods and gram (+) cocci, so Augmentin or Cipro+Flagyl or a cephalosporin+Flagyl are reasonable choices.
Of course, a patient can refuse drainage, and ask to try antibiotics to see if that will resolve the problem. It is a patient’s choice how to proceed, but it is important that you offer them the best and quickest way to treat this. Also, if your surgeon disagrees that drainage is needed, at least you have done everything appropriately, and hopefully the surgeon will follow the patient until this is resolved.
Are antibiotics always necessary?
Antibiotics are probably not absolutely necessary in most situations if adequate drainage has been performed. However, they might decrease pain, inflammation, and fever more quickly. Cultures are not necessary if adequate drainage has been accomplished. If you are going to put a patient on antibiotics, coverage for anaerobes along with gram (-) rods and gram (+) cocci makes logical sense, so Augmentin or Cipro+Flagyl, or a cephalosporin+Flagyl are reasonable choices.
What happens after the abscess is drained?
This is another point in the patient’s care where the ball is often dropped. Once the abscess has been drained and the patient has recovered, it is important to have a conversation regarding what to do next. For many patients, this conversation never occurs, and they are under the impression that their “pilonidal cyst” has been treated and cured. Unfortunately, this is not the case. These patients have at least a 50% chance of having another abscess or developing a pilonidal sinus, and they should be given the option of having a more definitive operation to prevent this from happening. This conversation should occur between the patient, possibly the patient’s family, and a surgeon who is confident and experienced in the treatment of pilonidal disease.
There is controversy regarding how aggressive to be in this situation. In our clinic, since we have a 99% success rate when we perform a cleft lift on these patients, we can be confident that this is a good solution. If a surgeon only performs excisional operations, the reported success rates are in the 33-50% range which makes aggressive excision less logical.
My recommendation is that the patient is referred to a surgeon who frequently and successfully performs the cleft lift operation, or is referred to this website www.pilonidal.com for more information.

